Table of Contents
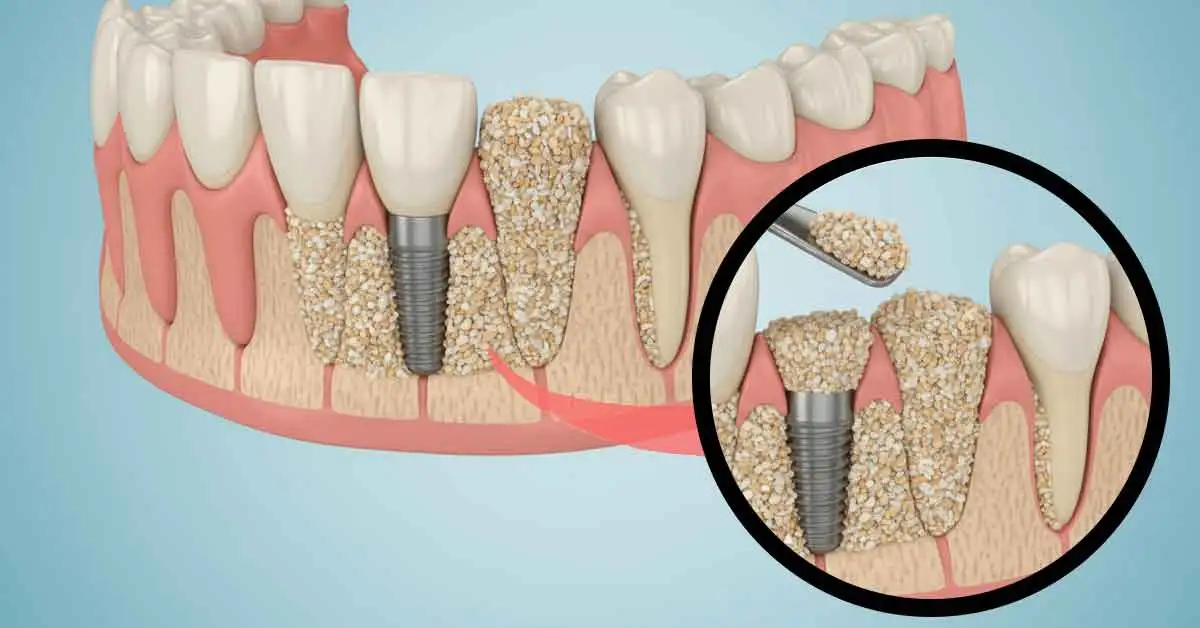
ToggleAfter tooth extraction, rapid bone resorption begins, and the solid foundation for an implant may be lost. This is where the answer to the question “What are bone grafts and PRF?” comes into play. Grafts fill the void and build a scaffold; PRF is prepared from your own blood, accelerates healing with growth factors, and seals the tissue. When used with the correct indication and sterile surgery, bone volume is preserved, soft tissue quality improves, and the long-term stability of the implant is strengthened.
Bone graft; What is PRF? Basic definition and logic
Bone graft is a graft material used to replace lost volume and guide new bone formation. PRF (Platelet-Rich Fibrin) is a fibrin mesh obtained by centrifugation, rich in platelets and leukocytes; it biologically activates the area, increases blood flow, and holds the graft particles in place. This duo provides both mechanical stability and biological speed in the surgical field.
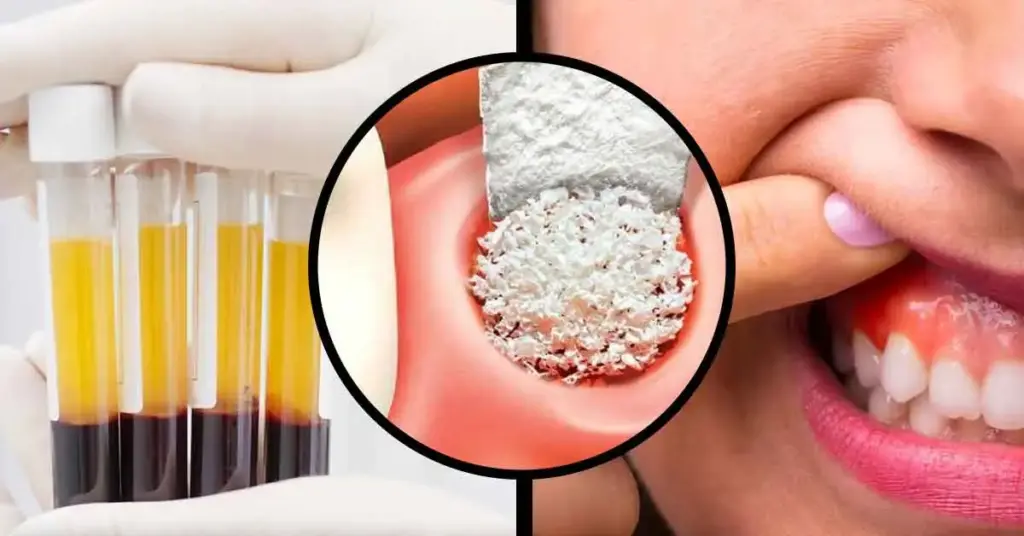
- Bone powder: Synthetic, animal-derived, human-derived, or autogenous options
- PRF: Prepared from the patient’s own blood during the same session
- Growth factors: Tissue repair is triggered by PDGF, TGF-β, and VEGF
- Fibrin membrane: Covers the graft and reduces micro-movement
- Expected outcome: More predictable bone formation and rapid epithelial closure
What are bone powder and PRF? In which cases are they used?
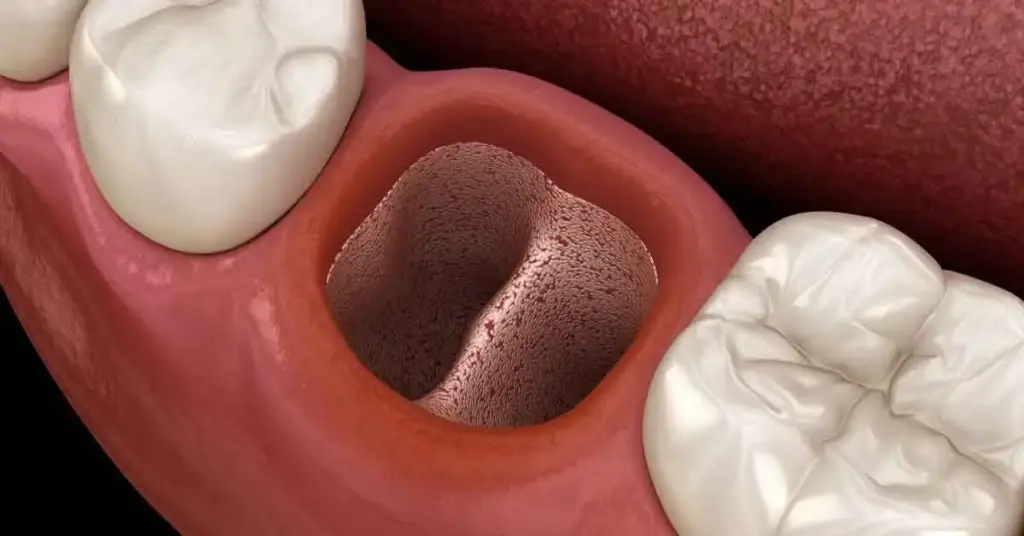
Not all extraction sockets heal the same way; the combination of graft and PRF makes treatment safe in cases of missing bone walls, proximity to the sinus floor, or post-cystic voids. It can be applied during the same session or during the preparation phase, depending on the implant plan.
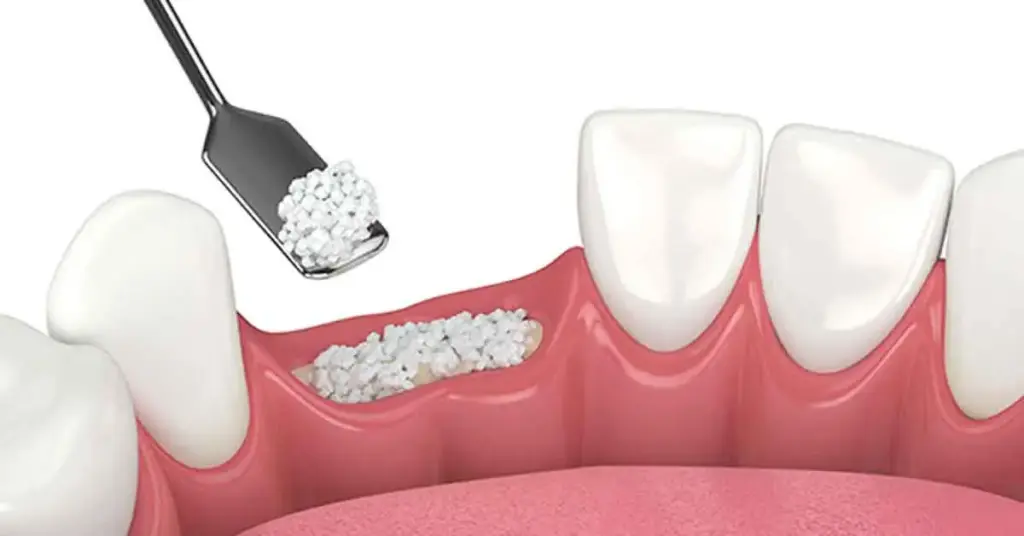
- Extraction socket preservation: To limit resorption and preserve the profile
- Sinus lift: Gaining vertical volume in the posterior maxilla
- Ridge augmentation: Thickening thinned ridges
- Peri-implant defects: Filling craters and notches
- Post-cyst/lesion: Regaining lost volume
What is bone grafting; PRF? Its relationship with implant success
Implant success depends on the triad of primary stability, sufficient bone volume, and healthy soft tissue. Graft volume is provided, PRF accelerates biological healing; thus, the osseointegration window is passed more safely, and marginal bone loss is kept under control.
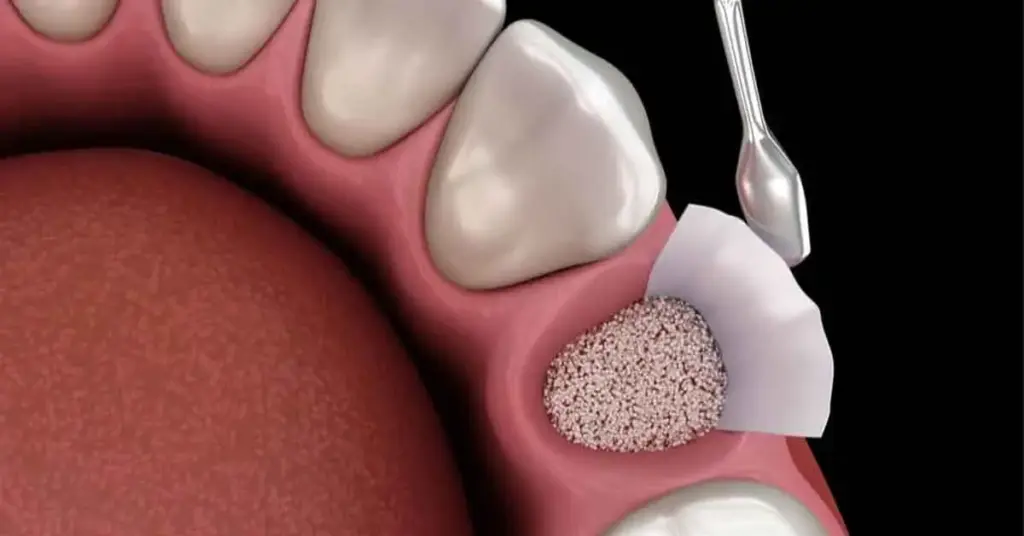
- Stability: Graft + PRF reduces micro-movement, preserves the clot
- Blood supply: PRF increases cell migration and nutrition
- Soft tissue: Thick, keratinized gingival contour is supported
- Infection control: Leakage and contamination are reduced with membrane coverage
- Long term: Bone levels are more stable in screw-retained superstructures
Comparison of graft types and PRF
Graft material works alone; however, when used with PRF, adhesion, patient comfort, and wound closure are significantly improved. The choice is made based on the volume of the defect, the number of walls, and the patient’s systemic condition.
- Autogenous graft: “Gold standard”; requires a second surgical site
- Allograft: Good volume and moderate resorption rate
- Xenograft: Slow resorption; provides long-term scaffold function
- Synthetic (β-TCP, HA): Sterile, predictable; easy particle control
- Combination: Graft + PRF gel/membrane = stability and rapid closure
Application process, healing, and potential risks
Treatment is planned using CBCT and clinical examination. The graft is placed under local anesthesia, covered with a PRF membrane, and primary closure is achieved. The implant is placed either during the same session (immediate) or 3–6 months later, depending on the case. Regular check-ups, oral hygiene, and smoking restrictions directly affect the results.
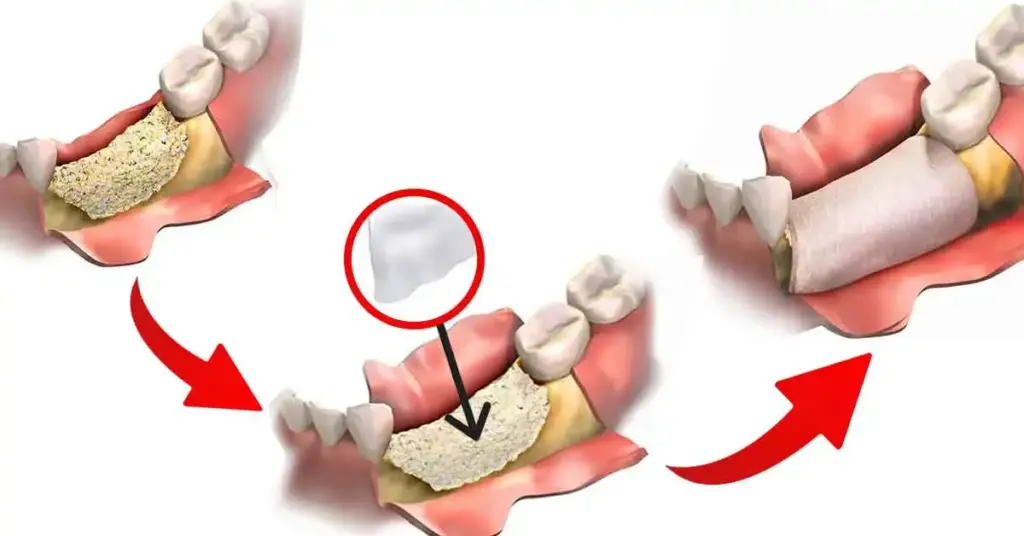
- Steps: Planning → blood collection and PRF → grafting → PRF closure → suturing
- Comfort: PRF may help reduce pain/swelling
- Duration: Osseointegration generally takes 12–24 weeks
- Care: Gentle brushing, antiseptic mouthwash, avoiding trauma
- Possible risks: Infection, suture opening, graft loss; early intervention is important
Check out our social media and smile gallery for perfect dental results.
Bone Grafts: Frequently Asked Questions
Is PRF or bone powder more important?
They play different roles. Bone powder establishes the site with its volume and framework; PRF provides biological acceleration. Using both together increases success rates in most cases.
Is PRF natural? Does it cause allergies?
PRF is prepared entirely from your own blood. Allergies are not expected. It is safe as it is produced under sterile conditions.
When can I have an implant after the graft?
It depends on the size of the defect and the quality of the bone. In most patients, the implant is placed 3-6 months later; in suitable cases, it is possible during the same session.
Is the procedure painful, and how is the recovery?
It is comfortable under local anesthesia. Since PRF covers the wound surface, pain and swelling are generally milder. Following your dentist’s medication and care recommendations speeds up recovery.