Table of Contents
ToggleTooth sensitivity is a sudden, brief but sharp pain triggered by hot, cold, sweet, or acidic stimuli. Most people describe it as a “needle prick” and it usually concentrates on one or two teeth. This condition occurs due to enamel thinning and exposure of dentinal tubules; in other words, when the protective shield weakens, the stimulus reaches the nerve endings directly. As tooth sensitivity progresses, triggers increase, daily eating and drinking enjoyment is disrupted, and even brushing becomes a problem. Small measures taken early on and the right products provide relief in most cases without the need for clinical treatment. If the complaint persists, an examination is necessary to rule out underlying causes such as decay, cracks, or gum recession.
Tooth Sensitivity: Symptoms and When Does It Occur?
Tooth sensitivity manifests itself during the day with minor contact; the first sip of cold water in the morning, ice cream in the evening, or sometimes even a hard brush stroke is enough. The pain usually lasts for seconds but is recurrent; after a while, the person memorizes which tooth is “triggered.” If throbbing is added during biting or chewing, a crack or high filling should be considered. Prolonged pain that wakes you up at night indicates pulp involvement beyond sensitivity. In short, duration and intensity provide important clues in understanding the underlying problem.

- Sudden, short stinging pain
- Pain that increases with cold/heat, triggered by sweet/sour foods
- Sensitivity when brushing or flossing
- Localized sensitivity in specific teeth
- Pain that wakes you up at night requires urgent attention
Causes of Tooth Sensitivity: Enamel Wear, Gum Recession, Cavities
The root cause of tooth sensitivity is the opening of dentinal tubules due to weakening of the enamel and cementum. Hard brushing, acid erosion, or teeth grinding thin the enamel; receding gums leave the root surfaces vulnerable. Cavities and microscopic cracks facilitate the passage of stimuli to the nerve. Home whitening treatments can also cause temporary sensitivity; this is due to increased surface permeability and can be controlled with the correct protocol. Identifying the underlying cause is the only way to choose the right treatment.
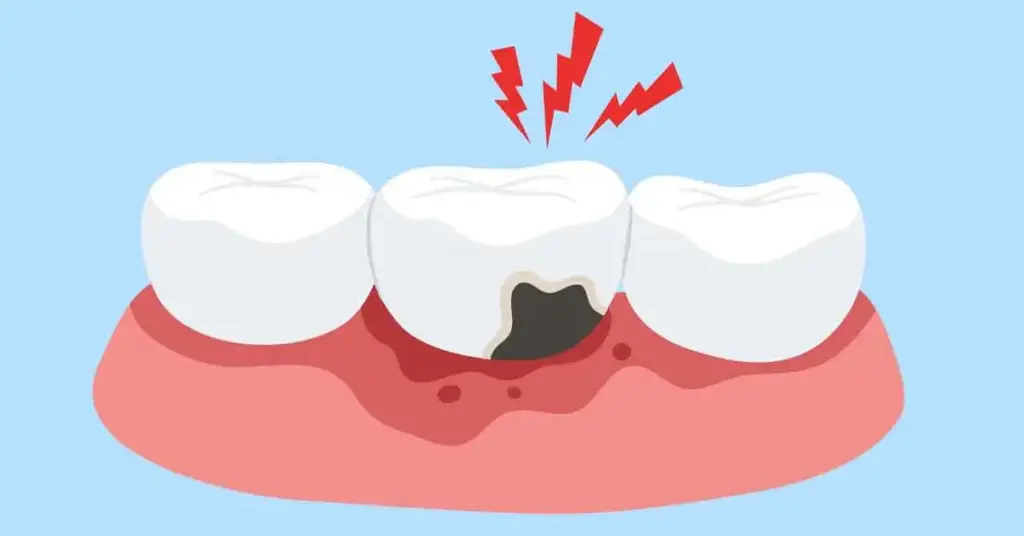
- Abrasive brushing, hard-bristled brush
- Acidic drinks, reflux, frequent snacking
- Bruxism (night clenching) and enamel microcracks
- Exposure of root surfaces due to gum recession
- Decay, old filling leakage, cracked tooth
- Temporary sensitivity after whitening or periodontal procedures
Diagnosing Tooth Sensitivity: When to See a Dentist?
A definitive diagnosis is made through clinical examination and radiographic evaluation; however, controlled observations that can be done at home shorten the path to seeing a dentist. Targeting a specific tooth with a cold water test helps to understand whether the complaint is localized or widespread. If you see wear grooves or a recession line in the neck area of the tooth in the mirror, your brushing technique should be reviewed. Do not delay an appointment if you have pain lasting longer than 1–2 weeks or increasing in severity, pain that wakes you up at night, or a sharp stabbing sensation when biting. Early diagnosis means minimal intervention and quick relief.
- Cold water spot trigger test
- Check for wear/retraction in the neck area with a mirror and light
- Morning jaw fatigue (sign of bruxism)
- Appointment for complaints lasting longer than 1–2 weeks
- Emergency evaluation for pain that wakes you up at night or occurs spontaneously
Treatment Options and Daily Care for Tooth Sensitivity
The goal of treatment is to close open dentinal tubules, calm the inflammatory response, and reduce triggers. The first step is usually topical solutions: pastes containing potassium nitrate or stannous fluoride suppress nerve conduction and block the tubules. In clinical practice, fluoride varnishes, high-fluoride gels, and desensitizing agents seal the surface. In cases of neck wear, root surfaces are re-isolated with bonding or composite restorations. If there is a crack, significant material loss, or pulp involvement, more advanced restorations or root canal treatment may be indicated. For bruxism, a custom-made night guard and stress management are essential; otherwise, all gains will be lost in a short time.

- Desensitizing paste: twice daily, for at least 4–8 weeks
- Fluoride varnish/gel: periodic applications in the clinic
- Bonding/composite: for exposed dentin and neck abrasions
- Repair or crown options for cracks/fractures
- Root canal treatment for pulp involvement
- Night guard + habit management for bruxism
Prevention and Nutrition Recommendations to Reduce Tooth Sensitivity
Prevention is as important as treatment, because daily habits determine the fate of tooth sensitivity. A soft-bristled brush and gentle circular technique quickly reduce neck wear. If you frequently consume acidic beverages, rinse with water after drinking and delay brushing for 30 minutes; otherwise, softened enamel will wear away more quickly. Limit frequent snacking; xylitol gum increases saliva flow and balances pH. Adding floss and an interdental brush to your routine reduces inflammation at the gum line, which slows recession. Regular scaling and check-ups keep the situation stable.
- Soft brush, light pressure, circular motion
- Rinse with water after acidic drinks, delay brushing for 30 minutes
- Reduce frequent/sugary snacks, use xylitol gum
- Add dental floss and interdental brushes to your daily routine
- Consider a night guard if bruxism is suspected
- Professional care and education every 6 months
Tooth Sensitivity – Frequently Asked Questions
Does tooth sensitivity go away completely?
In most cases, yes; it decreases significantly with proper diagnosis and regular application. Desensitizing toothpastes begin to take effect in 2–4 weeks, peaking at 8 weeks. If the underlying cause is not corrected (e.g., bruxism, acid erosion), the complaint will return. Therefore, product + habit change should be carried out together.
Which toothpaste really works?
Potassium nitrate targets nerve transmission, while stannous fluoride targets tubule openings; both are clinically supported options. Regular and long-term use is critical; a weekend-off, Monday-start approach will not yield results. Spitting out the toothpaste after brushing and not rinsing the mouth thoroughly with water increases its effectiveness.
Is tooth sensitivity normal after whitening?
Yes, temporary sensitivity is common and usually subsides within 24–72 hours. Remineralizing products before the procedure, intermittent application on treatment days, and fluoride varnish afterward provide relief. If the discomfort is severe, the concentration, duration, and frequency should be reevaluated with your dentist.
When should I be concerned and schedule an appointment immediately?
If the pain wakes you up at night, if biting causes increased pain, if the pain is concentrated in a single spot, or if it lasts longer than two weeks, do not wait. There may be a fracture, crack, deep decay, or pulp involvement. Early intervention often prevents the need for advanced treatments, from simple surface sealants to more complex procedures.

